 |
| Z I M - Paper 14th PCS/E Manchester |
Oct. 1998
Last update: 11.11.1998 |
Multidimensionality
|
Wolfram Fischer
Zentrum für Informatik und wirtschaftliche Medizin
CH-9116 Wolfertswil SG
(Switzerland)
http://www.fischer-zim.ch/
In: Proceedings of the 14th PCS/E International Working Conference. Manchester 1998.
|
|
|
|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||
INTRODUCTION: The development of patient classification systems (PCS) in fields other than acute medicine raises the question if the principle of using existing data (i.e. diagnoses; procedures where available) is sufficent to describe the products of hospital care.
METHODS/MATERIAL: The essence of a PCS (type "iso-cost") is to estimate costs of treatment needed in a defined setting by means of a description of the patient status (conditions) and the treatment goals. Two hypotheses guided our research into PCS development: (1) The description of patient status and treatment goals has to include multiple aspects which ideally are coded by using scales to show changes during the course of time. (2) In a multiprofessional team, costs of treatment of each professional sector can depend on different aspects of the patient status. Therefore, in a first step treatment costs could be described multidimensionally: for each profession sector separately. - In a test study, 1795 treatment weeks of 274 patients of 4 medical rehabilitation institutions were described by a variety of patient status indicators.
RESULT: The test study showed that the sum of nursing times per week and patient were best grouped by a two-dimensional grid constructed by using the motor scale and the cognitive scale of the Functional Independence Measure (FIM). These scales are used as indicators of the patient status. The six final groups lead to a variance reduction of approx. 65%. But the time spent by several therapeutic professionals could not be explained by the same indicators.
CONCLUSIONS: The test study encourages further research about the introduction of multidimensional and scaled measures in order to explain the multidimensional cost vectors of a multiprofessional health treatment. In the acute setting a first model could be to use DRGs to estimate costs related to or dependent on physicians' activities and a measure of functional status to estimate (independent) nursing costs. A proposed research field is the treatment of patients with chronic diseases.
The development of patient classification systems (PCS is
normally restricted by the obligation to use existing data. The results
are interesting. But if we look at them with the eyes of a statistician
we must say they are not very convincing. As indicator for the goodness
of the grouping result, the reduction of variance of costs or length
of stay is often used. The most detailed one-dimensional PCS for acute
stays is probably the APR-DRG system. 3M - the
owner of APR-DRG - has published an overall reduction of variance of 53%
on american data for untrimmed charges (see table below).
This is a higher value than other systems can present;
but from the statistical viewpoint this value
is still clearly below the limit of 75% for good values.
| Untrimmed length of stays | Untrimmed charges (bill amounts) | |||||
|---|---|---|---|---|---|---|
| All | Medical | Surgical | All | Medical | Surgical | |
| HCFA-DRG | 31% | 29% | 33% | 41% | 25% | 41% |
| SR-DRG | 34% | 30% | 38% | 44% | 27% | 45% |
| RDRG | 37% | 35% | 38% | 46% | 35% | 46% |
| AP-DRG | 37% | 36% | 37% | 47% | 37% | 45% |
| APR-DRG | 42% | 38% | 45% | 53% | 42% | 52% |
Table
1:
Variance reduction (R2) of several DRG systems [1]
Still today we have lower values for medical groups compared to surgical
groups, particularly if we look at the results for charges. That shows
that diagnoses are a weaker grouping criterion than procedures. Knowing
that PCS should derive groups which are classified relating to the
ressources needed, an ideal PCS would use patient status
(conditions) and preferably also treatment goals as grouping criteria,
but not treatment characteristics. Diagnoses meet this demand;
procedures - which produce better results - do not.
These observations and the development of PCSs in fields other than acute medicine, where fewer data is available, raise the questions:
The essence of a PCS (type "iso-cost") is to estimate costs of needed treatment in a defined setting by a description of the patient status (condition) and the treatment goals. Two hypotheses guided our research into PCS development: (1) The description of patient status and treatment goals has to include multiple aspects which ideally are coded by using scales to show changes during the course of time. (2) In a multiprofessional team, costs of treatment of each professional sector can depend on different aspects of the patient status. Therefore, in a first step, treatment costs could be described multidimensionally: for each profession sector separately.
In a test study, 1795 treatment weeks of 274 patients of 4 medical (neurological) rehabilitation institutions were described by a variety of patient status indicators (1716 of them had evaluable nursing data). [2] [3] This was done as part of the work of a project called "TAR" ("Leistungsbedarfsbezogenes Tarifsystem für Rehabilitationskliniken" = reimbursement system for rehabilitation clinics oriented to needs of treatment). In this paper parts of the TAR PCS will be presented. Other planned elements of TAR are certification, guidelines, reporting system and a reimbursement model which is based on all the other compoments. The hypothesis is that additional data should cover patient status (condition) and possibly also treatment goals but not treatment characteristics.
The following indicators for the need of treatment were evaluated in the first survey: main rehabilitation diagnostic groups, impairment, disability (mainly Functional Independence Measure (FIM) [4] with additional assessments in order to refine lower and upper edge zones), selected social burdens, description of the rehabilitation treatment segment, the main rehabilitation goals, the main rehabilitation obstacles. (The last two items were neither coded nor evaluated in the first evaluation cycle.)
As dependent variables, nursing and therapeutic times were collected for each day in order to calculate variable costs and to construct typical ways of treatment.
The data was united in a relational database. The evaluation comprised a multitude of CART [5] calculations done with the help of the Systat program [6]. The final version of the grouping for nursing costs was derived from the statistical outputs by discussing them with physicians.
The best results were found for nursing times when explained by the motor scale and the cognitive scale of the Functional Independence Measure (FIM). But we could not find any relevant and meaningful relation between any item of the patient condition and the therapeutic times.
Therefore I will only present some results from the nursing classification. It is presented here as a prototype element of a multidimensional classification approach.
The FIM™ instrument
(Functional Independence Measure) [4] is a
sort of a ADL (Activities of Daily Living) measure, complemented with items
for cognitive disability. It comprises 18 items, each evaluated on a 7
point ordinal scale which indicates a range from full independency to
total independency of help assistance needed.
(Using the FIM™ instrument is mandatory
in the american UDSmr = Uniform Data System for Medical Rehabilitation.)
| MOTOR ITEMS | Sum: 13 to 91 | ||
|---|---|---|---|
| A | Self/Care | Eating | 1 to 7 |
| B | Grooming | 1 to 7 | |
| C | Bathing | 1 to 7 | |
| D | Dressing - Upper Body | 1 to 7 | |
| E | Dressing - Lower Body | 1 to 7 | |
| F | Toileting | 1 to 7 | |
| G | Spincter Control | Bladder Management | 1 to 7 |
| H | Bowel Management | 1 to 7 | |
| I | Transfers | Bed / Chair / Wheelchair | 1 to 7 |
| J | Toilet | 1 to 7 | |
| K | Tub / Shower | 1 to 7 | |
| L | Locomotion | Walk / Wheelchair | 1 to 7 |
| M | Stairs | 1 to 7 | |
| COGNITIVE ITEMS | Sum: 5 to 35 | ||
| N | Communication | Comprehension | 1 to 7 |
| O | Expression | 1 to 7 | |
| P | Social Cognition | Social Interaction | 1 to 7 |
| Q | Problem Solving | 1 to 7 | |
| R | Memory | 1 to 7 | |
Table
2:
FIM Items [4]
The TAR nursing classification was designed according
to the evaluation of the data in two steps. FIRST a grid of three
categories of cognitive disability and four categories of the
motor and practical disability were constructed. This led to 12
so called "TAR FIM base classes".
| Cognitive Disability | |||||
| very severe | medium to severe | minimal to little | |||
| Cogn. FIM 5-10 |
Cogn. FIM 11-29 |
Cogn. FIM 30-35 |
|||
| Practical / Motorical Disability | very severe | Mot. FIM 13-26 |
Twelve clinically relevant combinations |
||
| severe | Mot. FIM 27-55 |
||||
| medium | Mot. FIM 56-80 |
||||
| minimal to little | Mot. FIM 81-91 |
||||
Table
3:
TAR FIM base classes [3]
Legend:
- Mot. FIM: Sum of FIM-Items A to M
- Cogn. FIM: Sum of FIM-Items N to R
In a SECOND step these 12 possibilities of combinations were joined
into six groups with similar average nursing times. The six final
groups led to a variance reduction of approximately 65%.
| Categories of nursing costs | Cognitive Disability | ||||
|---|---|---|---|---|---|
| very severe | medium to severe | minimal to little | |||
| Cogn. FIM 5-10 |
Cogn. FIM 11-29 |
Cogn. FIM 30-35 |
|||
| Practical / Motorical Disability | very severe | Mot. FIM 13-26 |
P6 | P5 | P4 |
| severe | Mot. FIM 27-55 |
P5 | P4 | P3 | |
| medium | Mot. FIM 56-80 |
P2 | |||
| minimal to little | Mot. FIM 81-91 |
P4 | P1 | ||
Table
4:
Categories of nursing costs [3]
Legend:
- Mot. FIM: Sum of FIM-Items A to M
- Cogn. FIM: Sum of FIM-Items N to R
| P1 | P2 | P3 | P4 | P5 | P6 | Overall result | ||
|---|---|---|---|---|---|---|---|---|
| Nursing Hours per Day | Median | 0.9 | 2.5 | 3.5 | 4.9 | 6.3 | 8.6 | 2.4 |
| Average | 1.1 | 2.7 | 3.8 | 5.4 | 6.6 | 9.0 | 3.5 | |
| Coefficient of Variation | 0.69 | 0.54 | 0.43 | 0.42 | 0.44 | 0.32 | 0.93 | |
| Nursing Weeks | 714 | 269 | 170 | 256 | 157 | 150 | 1716 | |
Table
5:
Statistical values from the categories of nursing costs [3]
These results are preliminary results of a first survey. The coefficent of variation is below 0.5 in nearly all groups. This is good compared to the commonly accepted limit of 1.0 in the field of PCS. Several analyses of the test data set showed that the results are relatively stable.
It is now necessary that this classification and its statistical values are tested in further sets of clinics. Also the classification must be rebuilt in other domains of rehabilitation e.g. rheumatic rehabilitation, orthopedic rehabilitation, geriatric rehabilitation. I would not be astonished if the values and/or the system of aggregation of the base classes would change. It must be studied if further criteria of disability or handicap has relevant influence for other rehabilitative treatment types or in other settings.
But what I want to discuss here is the approach. The relatively high reduction of variation through only six groups encourages me to discuss the potential reasons for this first success.
At first sight I suppose that the chosen grouping criteria seem to be fairly appropriate to predict the dependent variable in this environment. Therefore I want to discuss the question:
FIRST the two used FIM scales are indicators of the patient status; they are not based on treatment. We describe a facet of the condition of the patient and we say nothing about what the provider has done. The latter is solely quantified by the dependent variable which was in this study the sum of the measured nursing times per week divided by seven (days).
SECOND the FIM scales are scales. Scales allow us to differentiate more flexibly than yes-no-categories. An example for yes-no-categories are diagnoses of physicians. Scales enable us to follow the development of the patient status in the course of time. Moreover using scales to describe patient status allows us to use it not only to describe the current state but also to describe goals and outcomes (i.e. state to achieve resp. state achieved). [8]
THIRD the FIM scales describe the patient status beyond the phyisicians' view of diagnoses. It is essential to realize that for treatment in certain settings other criteria than diagnoses of physicians can predict costs better. In our case, we found variables which were used by all members of the treatment team. Above all it encompasses also parts of the view of nurses and therapists.
FOURTH we used days and not cases as treatment units. This could be a handicap if we want to use this classification for reimbursement. But if we understand this classification as a module of a multidimensional classification system we can use it either for reimbursement per diem or for reimbursement per case. If we want to construct a system to pay for cases, we know that nursing costs of each day in neurological rehabilitation are dependent on the disability of the patient. Reimbursement per case would work with the hypothesis of a standardized development of the disability during the stay and a planned average length of stay. Now we could easily calculate nursing costs of the stay by using the presented classification of nursing costs per diem. We have to know that for certain applications inside the clinic we prefer a detailed classification, e.g. for planning the nursing work or for quality control.
FIFTH we can suppose that the chosen independent variables are special for this environment although I would be very much interested to see if the same variables could also be used in other settings. That means that besides the definition of classification criteria there must be a description of the required treatment environment, the setting. This can lead to the demand of certification of the institutions as a prerequisite for reimbursement contracts.
SIXTH in the example study we did not use treatment goals to classify nursing costs. It could be that one of the reasons, why we were not successful in grouping therapeutic times by means of the same list of patient status items, is that we were not able to quantify treatment goals.
SEVENTH in the example study we did not differentiate between primary and secondary problems i.e. on the one hand conditions (and related treatment goals) that justify the hospital stay on the other hand additional conditions which are not in the center of the treatment but nevertheless do increase treatment intensity and resource use. It seems that the disability items as descibed by FIM encompass the two types of problems at least partially. We need not know e.g. the reason why a patient is not able to eat without help. It is not relevant if this disability is caused by the problem the patient is treatet for or by another (preexisting) problem of the patient. Nurses will perform in both cases what is necessary. But the question of problem types gains another relevance if we were to use e.g. diagnoses as grouping criteria. We must know if they are part of the description of the primary problem and are treated until a certain (primary) goal is achieved or if they belong to secondary problems which are treated only while the primary goal is not achieved or which are not treated. Examples of diagnoses which could belong to secondary problems are diabetes mellitus, adipositas, blindness, dementia, disorientation, incontinence, decubitus and so on.
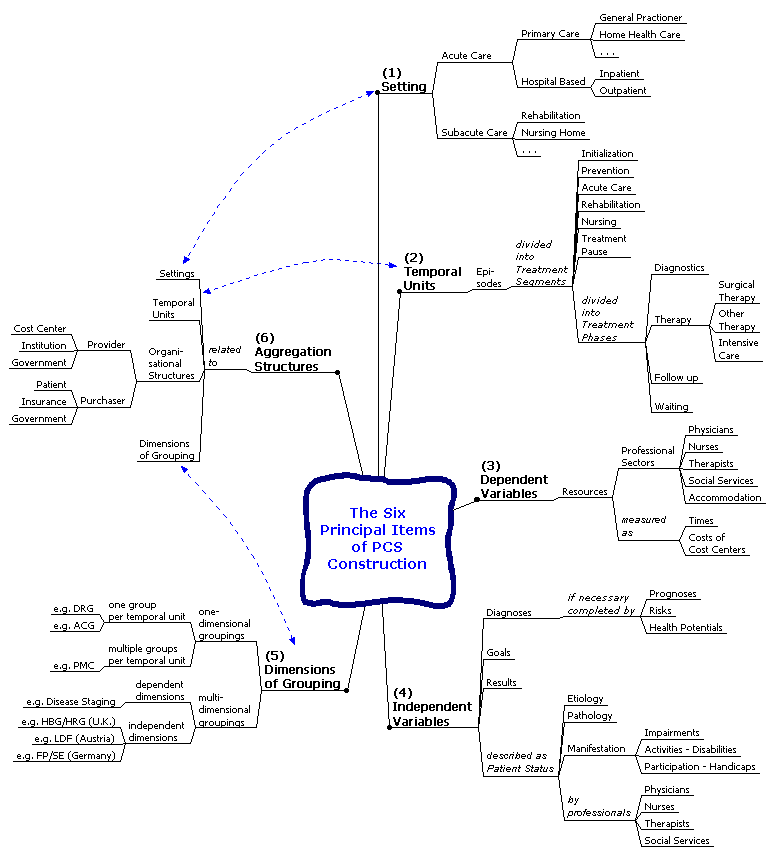
From all that we could derive the principal items nessessary for the construction of a multidimensional patient classification system.
To build a PCS, the FIRST STEP is the description of the aim that the PCS should fulfill. the SECOND STEP is the choice and definition of construction principles and elements. The THIRD STEP is the definition of its contents. The FOURTH STEP is defining and calculating cost weights and other figures like trim points.
In this paper, only the second stop will be discussed: the choice and definition of construction principles and elements of a PCS. Regarding this step, we must consider the following six principal items:
 |
Table
6:
The six principal items for PCS construction
If the setting is described precisely, it will help a great deal to derive appropriate and operational certification criteria.
The setting should be described in such a manner that the resulting PCS can be integrated into aggregations structures which overlap several settings.
An appropriate and exact definition of the temporal units in the course of treatment is very difficult. E.g. in the hospital environment the so called "case" lasts from admission to discharge. This leads to a rather vague and inhomogeneous grouping of processes belonging to a case. What will be done if the patient changes a hospital division or if he changes for the same reason from one hospital to another? Is there a difference between a case discharged to go home or to a nursing home?
As an approach to obtain a structure of time, episodes can be partitioned into treatment segments with different goals and these again into treatment phases with different treatment approaches. [2] [7]
The dependent variable for a PCS of the type "iso-costs" will be costs. It can be quantified by measuring activity times as a reference quantity or by the calculation of costs.
The independent variables are the grouping criteria. They should describe the current patient status, probably also the treatment goals which can be seen as the patient status aimed at and perhaps also results which can be seen as the patient status achieved after the treatment. So the same language and coding could be used. [8]
Although the result (outcome) is nowadays one of the preferred criteria (but not very often implemented), we should be aware that the results in terms of regained health is not the choice of top quality in every setting. E.g. in the rehabilitation setting it is possible that an agreement is made upon a particular treatment of a patient in coma over a certain length of time without fixing a certain outcome. This could be done simply because there is a - perhaps slight - chance to achieve a better patient status. The outcome will not be relevant to the payment of this treatment but to the decision about the treatment that will follow.
The main stream of inpatient PCS development found consensus in the premise that one temporal unit should be covered by one patient category. [9] There are exceptions such as Patient Management Categories (PMC) or Disease Staging. [10] [11] [12] Also in the German system you can assign multiple cost weights to one case. [13] In the Austrian system which is in practical operation since 1997 you can assign more than one characteristic to one case: one or - in certain cases - more than one patient group called LDF (Leistungsbezogene Diagnose-Fallgruppen = performance-related diagnostic case groups) and, supplementary, the count of days of intensive care. [14] The most interesting alternative approach is the twofold approach of the HBG/HRG-matrices in the U.K. [15] [16] [17]
In fact, the instruction to have only one patient category for one temporal unit is a manner to handle the financial risk (and to simplify statistics). It works if the treatment paths including the accessory goals are relatively well defined for each patient category. But if the treatment paths are dependent on many factors not known at the beginning of the treatment, it is not obvious that solely the provider should carry this financial risk. It could be wise to define groupings which enable flat (all-inclusive) payments but which could be combined to a certain extent. They will still be a further incentive regarding cost containment than many single fees for services but they can also be more fair regarding the distribution of financial risks.
To construct a multidimensional PCS the easiest way is to analyse the
costs and temporal units of each professional sector. It is possible to
detect that we can use the same independent variables in each sector. But
it is more probable that we will find diffent criteria as cost drivers. In
multidimensional classification systems the number of groups for each
professional sector will shrink. (E.g. in the example presented before
we were able to explain costs per diem for the nursing sector rather
satisfactorily with only six groups.) The result of such an analysis
will be several classifications, each with a restricted number of groups.
They can be based on different temporal units.
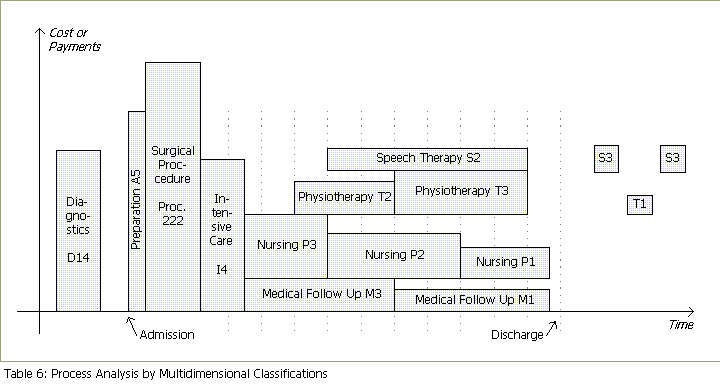 |
Table
7:
Example of a process analysis by multidimensional classifications
The real art of PCS construction will begin now: Which professional dependent classifications can be aggregated into one single classification? (Systems like DRGs have put everything - except physicians' activities - together into one classification. [9]) The challenge behind the problem is to agree about which parts are dependent on the main treatment process and which parts should be prescibed independently of the main process. This problem is linked to the dilemma of target values versus current values.
Aggregations can be made by aggregating dimensions of groups, joining temporal units, settings and/or organisational structures of providers or purchasers.
To decide about aggregation we must FIRST know which processes are dependent on which others. E.g. is intensive care (statistically seen) strongly related to a certain surgical procedure? Is nursing dependent on a medical treatment cycle? Are nursing costs and therapy costs correlated? (In our rehabilitation project we found that nursing costs are independent of therapeutic costs and the latter cannot be explained by the same grouping criteria.)
SECOND we must decide which values should be defined as standards and which values should be measured during each treatment. E.g. "Nursing P3" with cognitive FIM between 30-35 and motor FIM between 27-55 has a standard time of 3.8 hours per day. Supposing post-operative nursing activities are directly dependent from "Proc. 222" we can define a standard duration for "Nursing P3 in combination with Proc. 222" of e.g. 3 days. In this case, the cost weight of "Nursing P3" would a component of the cost weight of "Proc. 222". Another possibility could be: The post-operative patient status is not very strongly correlated to "Dg. X" treated by "Proc. 222", i.e. there is a rather big range of disabilities measured by FIM after the application of "Proc. 222". Consequently we should allow that the post-operative nursing categories can be described as the current patient status determined once each week during the rest of the stay.
THIRD we must be aware that the aggregation process can vary for internal applications and for external tasks. It would be very helpful if we could invent a system which can be aggregated resp. differentiated according to the type of application. E.g.: Suppose that in regard to reimbursement we could agree upon aggregating all cost components and classifications into one single classification describing hospital cases or other types of episodes. In terms of cost accouting we would sell one product per temporal unit. We can call it the profit-relatable production units. On the other hand, the cost-relatable production units would be the professional-oriented categories aggregated at a lower level than the profit-relatable production units.
FOURTH: Knowing about the structure of the process and being able to describe it with a few professional-oriented classifications would help to arrive at a description of the products, which is missing until now in most systems. (An exception are the Patient Management Paths [PMP] of the PMC system.) It is a strange thing that in the health sector we try to define product lists by PCS construction, we assign prices to each product on the list, but we say nearly nothing about what will be done or what could be expected by buying/applying these products. A rough description would help to compare offers of different providers for the "same" product. Depending on how the description is made it could also reveal quality aspects. It would pave the way to discuss about goals of treatment regarding single patients and whole settings.
A test study in which other than conventional grouping criteria were analysed has encouraged us to further reflect and to continue our research into the introduction of multidimensional and scaled measures in order to explain the multidimensional cost vectors of a multiprofessional health treatment. In a setting with multiprofessional teams e.g. in rehabilitation, bundling of treatment activities can not only be done by using physicians' criteria. It is probable that will we have to use different criteria and/or classifications for different professional sectors if they are not very directly dependent on the physicians' activities. The latter is often assumed for surgery cases. But also in this setting we must discuss the new approach for patients with secondary problems which do increase the intensity of treatment and the use of resources. In particular it must be discussed in settings other than acute surgery.
In the acute setting a first model could use DRGs to estimate costs related to or dependend ont the physicians' activities and as a measure of functional status to estimate (independent) nursing costs.
Beyond that, the treatment of patients with chronic diseases by different providers, the typical area for the application of techniques of "disease management", will be an excellent challenge for the development of multidimensional PCS.
[1] Averill RF, Muldoon JH, Vertrees JC, Goldfield NI, Mullin RL, Fineran EC, Zhang MZ, Steinbeck B, Grant T: The Evolution of Case Mix Measurement Using Diagnosis Related Groups (DRGs). 3M HIS Working Paper 5-98. Wallingford 1998 (3M): 40 pp.
[2]
Fischer W:
Design Principles for an Inpatient Rehabilitation Patient Classification System.
In: Proceedings of the 13th PCS/E International Working Conference.
Florence, 1997:227-9.
Internet: http:// www.fischer-zim.ch / paper-en / PCS-Reha-Design-9710-PCSE.htm.
[3] Fischer W, Blanco J, Mäder M, Zangger P, Conti FM, Bapst L, Huwiler B: Patientenklassifikation in der Rehabilitation - Das neue TAR-Projekt. In: KSK-aktuell 4/1998: p. 60-62.
[4] Granger CV, Brownscheidle CM: Outcome Measurement in Medical Rehabilitation. International Journal of Technology Assessement in Health Care 11:262-8,1995.
[5] Breiman L, Friedman J, Olshen R, Stone C: Classification and Regression Trees. Belmont 1984 (Wadsworth). [ CART = Classification and Regression Trees ].
[6] SPSS: SYSTAT Version 7.0.1. Chicago 1997 (SPSS Inc.).
[7]
Fischer W:
Patientenklassifikationssysteme zur Bildung von Behandlungsfallgruppen im stationären Bereich - Prinzipien und Beispiele
(Patient Classification Systems for Grouping Hospital Cases
- Principles and Examples).
BSV and Z/I/M, Bern and Wolfertswil 1997: 514 pp, cit. p. 55-61.
See also: http:// www.fischer-zim.ch / auszuege-pcs-buch / Strukturierung-von-Behandlungsverlaeufen-9701.htm.
[8]
Fischer W:
PCS and Casemix Types.
In: Proceedings of the 11th PCS/E International Working Conference.
Oslo, 1995:50-7.
Internet: http:// www.fischer-zim.ch / paper-en / PCS-Types-9506-PCSE.htm.
[9] Fetter RB, Brand A, Dianne G [Eds.]: DRGs, Their Design and Development. Health Administration Press, Ann Arbor 1991: 341 pp.
[10] PRI: Patient Management Categories, Release 5.0. The Pittsburgh Research Institute, Pittsburgh, w/o year.
[11] Gonella JS, Hornbrook MC, Louis DZ: Staging of Disease. A Case-Mix Measurement. In: JAMA 1984(251)5:637-44.
[12] Gonella JS, Louis DZ, Marvin EG: Disease Staging: Clinical Criteria. Fourth Edition, MEDSTAT Systems, Ann Arbor 1994: 834 pp.
[13] Krankenhaus Umschau [Hrsg.]. ku-Sonderheft: Bundespflegesatzverordnung '95 mit Fallpauschalen- und Sonderentgeltkatalog inkl. 1., 2. und 3. Änderungsverordnung. Stand 18.12.95. Baumann, Kulmbach 1996: 78 pp.
[14] BMAGS-A: Bundesministerium für Arbeit, Gesundheit und Soziales: LKF 1998. Wien 1997.
[15] NCMO-UK: National Casemix Office: HBG - Health Benefit Groups Development Project. Information Sheet. Winchester, March 1996 (NCMO): 6 pp.
[16] Sanderson HF, Anthony P, Mountney LM: Healthcare Resource Groups - Version 2. Winchester 1996 (NCMO: Occasional Paper No. 6): 15 pp.
[17] National Casemix Office: HRG - Health Resource Groups; Definitions Manual: Introduction. Crown, Winchester 1991: 126 pp.
Z I M
-
Zentrum für Informatik und wirtschaftliche Medizin
|
| Previous Paper: | Tables of Contents: | Next Paper: |
| PCS Design in Rehabilitation | English Papers | A Comparison of PCS Construction Principles |
| Navigations-Tabellen | ||
| Z I M - Hauptseite |
© Z I M
Source =
http://www.fischer-zim.ch/paper-en/Multi-Dimensional-PCS-9810-PCSE.htm
( latest compilation:
26.08.2011
)